
Medically Reviewed by Dr. Lee Hwee Chyen
MBBS MRCP (UK) FAMS (Dermatology)

Melanoma is a type of skin cancer that originates in the melanocytes, the cells responsible for producing melanin, the pigment that gives skin its colour. Unlike other skin cancers, melanoma has a higher potential to spread to other parts of the body and become life-threatening if not detected and treated early. Melanoma is known for its ability to occur in both heavily sun-exposed areas and areas typically protected from the sun.
Melanoma is distinct from other forms of skin cancer in several ways. While basal cell carcinoma (BCC) and squamous cell carcinoma (SCC) are more common, melanoma is more aggressive and likely to metastasize. This means it is more likely to spread to other body parts, including lymph nodes and internal organs, making early detection and treatment crucial.
Melanoma often appears as a new dark spot on the skin or a change in an existing mole. In contrast, BCC may look like a flesh-coloured, pearl-like bump or a pinkish patch of skin, while SCC often presents as a scaly or crusty growth.
While all skin cancers are associated with UV exposure, melanoma is also linked to intense, intermittent sun exposure and sunburns, especially in youth.
Melanoma, like many cancers, arises from a complex interaction of genetic and environmental factors that include:

Preventing melanoma involves strategies primarily focused on protecting the skin from excessive ultraviolet (UV) radiation, which is a significant risk factor for melanoma. Adopting these preventative measures can significantly reduce the risk of developing melanoma:
The ABCDE rule is a simple guide used to help identify the signs of a dysplastic mole or melanoma. It’s not foolproof and some melanomas may not fit these criteria. Any new or changing moles or skin lesions should be evaluated by a dermatologist who specialises in skin cancer detection, especially if they are accompanied by other warning signs of skin cancer.
One half of the mole or skin lesion does not match the other half in terms of size, shape, colour, or thickness.
The edges of the mole or lesion are irregular, ragged, notched, or blurred.
The color is not uniform and may include shades of brown or black, or sometimes patches of pink, red, white, or blue.
The spot is larger than 6mm across (about the size of a pencil eraser), though melanomas can be smaller.
Any change in the mole or spot over time, such as in size, shape, colour, elevation, or another trait, or any new symptom such as bleeding, itching, or crusting.
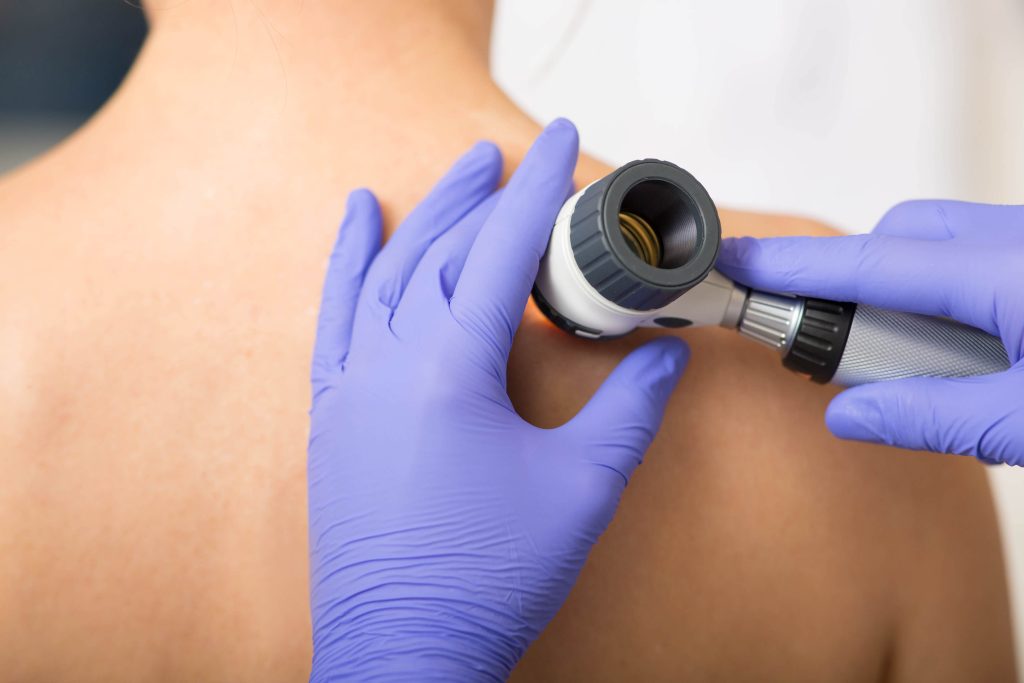
The process of diagnosing melanoma begins with a thorough examination of the skin by a dermatologist experienced in skin cancer. The specialist will check for moles, birthmarks, or other pigmented areas that look abnormal in size, shape, colour, or texture or are different from other spots on the skin.
A dermatoscope, a specialized instrument, may be used to look at skin lesions more closely. This tool provides a magnified, illuminated view of the mole, allowing for a more detailed examination.
If a mole or lesion appears suspicious, a biopsy is usually the next step. This involves removing all or part of the skin in question and sending it to a laboratory for analysis. The biopsy sample is then examined under a microscope by a pathologist. This examination helps in determining whether the cells are cancerous and, if so, the type and severity of the cancer.
If melanoma is diagnosed and there is a concern that it has spread, additional tests like lymph node biopsies, imaging tests or blood tests may be recommended to check for metastasis.
Treating melanoma effectively often depends on the stage of the cancer at diagnosis.
In the early stages, the primary treatment for melanoma is surgical removal. This involves excising the melanoma along with some of the normal skin around it (a margin) to ensure all cancer cells are removed. The size of the margin depends on the thickness and location of the melanoma.
If melanoma has spread to nearby lymph nodes, a procedure to remove these lymph nodes may be necessary.
Uses medications to stimulate the patient’s immune system to attack cancer cells more effectively. Immunotherapy has been particularly effective in treating advanced melanoma and for reducing the risk of recurrence.
For some melanomas, targeted therapy can be used. These are drugs that target specific genes or proteins found in cancer cells. For example, drugs that target the BRAF mutation, which is present in some melanomas, are used to block the growth and spread of cancer cells.
Although less common now with the advent of targeted and immunotherapy, chemotherapy might still be used in certain cases, especially when melanoma has spread to other parts of the body.
This treatment uses high-powered energy beams, like X-rays, to destroy cancer cells. Radiation therapy is sometimes used to relieve symptoms of melanoma that have spread to other parts of the body.
The stage of melanoma at the time of diagnosis is crucial in determining the prognosis. The stages range from Stage 0 (in situ) to Stage IV (advanced cancer). Earlier stages indicate cancer limited to the skin, while later stages indicate spread to lymph nodes, organs, or other body parts.
According to current data, the 5-year survival rate for melanoma detected at an early stage (localized stage) is about 99%. For regional melanoma, which has spread to nearby tissue or lymph nodes, the 5-year survival rate falls to about 66%. For distant-stage melanoma, where cancer has spread to other parts of the body, the survival rate is about 27%.
Other factors that can affect the prognosis include the thickness and ulceration of the melanoma, the age and general health of the patient, and the specific type of melanoma. Consult a trusted dermatologist to obtain an accurate outlook on your melanoma prognosis.
By staying informed about the signs, engaging in regular skin checks, and taking preventive measures, you can play a proactive role in your skin health and reduce your risk of melanoma. Consult with a skin cancer specialist for personalized advice and regular check-ups if you have any suspicious-looking and/or rapidly changing moles.
Skin cancers can vary in appearance. They might be small, shiny, waxy, scaly, firm, red, or have irregular borders. Any new, unusual growths or changes in existing moles should prompt a consultation with a qualified dermatologist.
Many wonder whether eczema can resolve without treatment. The answer depends on the individual's type of eczema, age, environmental factors, and overall health status. Read on to learn more about eczema and the appropriate management strategies for this condition.
Acne is a skin condition that can be exacerbated by certain cosmetic ingredients. Understanding these ingredients can help prevent acne flare-ups and maintaining healthy skin. Read on to learn more.